
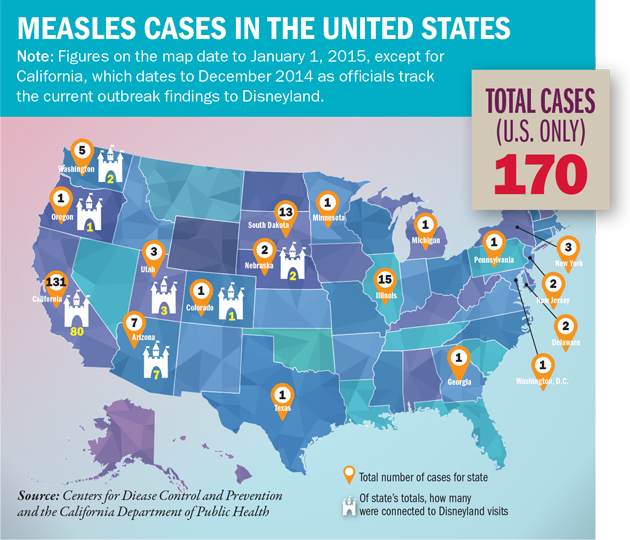
As of March 2, there were 131 reported cases of measles in California, 80 of which are directly tied to a December outbreak at Disneyland, according to the state Department of Health. Sixteen cases linked to the park have been confirmed in six other states, Canada and Mexico. Unrelated cases have popped up as well, impacting an additional 45 people from 10 states across the country, and prompting the quarantine of hundreds of children who may have been exposed at schools, hospitals and by family or friends.
Of the patients for whom officials could verify vaccination status, 82% had not been immunized for the measles, primarily because they intentionally declined, according to a January media briefing by Gilberto Chavez, deputy director of California’s state center for infectious diseases. A quarter of those infected have been hospitalized, and other cases likely have not been reported. “We can expect many more cases of this vaccine-preventable disease unless people take precautionary measures,” he said.
With a 99% efficacy rate, widespread vaccine coverage eradicated measles as an endemic disease in the United States in 2000, but travel to countries that still experience outbreaks and increasing non-compliance in the United States, United Kingdom, France and Canada have brought cases to a 20-year high. Measles remains one of the most infectious illnesses on the planet, with an infection rate of about 90% among unvaccinated people who are exposed. The virus stays active and contagious in the air for up to two hours, and it can be transmitted by an infected person up to four days before and after a rash ever develops. Before widespread vaccination, the virus killed 2.6 million people a year, according to the World Health Organization, and remains one of the leading causes of death among children worldwide. Indeed, it still kills 145,000 people annually—most of whom simply did not have access to the vaccine.
In the wake of the outbreak at Disney, schools and public health officials have been scrambling to contain the illness. Weeks after the initial news broke, health officials disclosed that at least five Walt Disney Parks and Resorts employees were also diagnosed with measles, two of whom had been vaccinated and three of whom were treated and medically cleared. Disneyland asked any employees who had not been vaccinated or could not confirm their immunity status to go on paid leave until their status could be confirmed.
Amid tremendous media attention, concerns have grown at other companies about how to mitigate the danger of the disease. For general employers outside the healthcare industry, current rules allow employers to provide information about outbreaks and relevant risks, encourage employees to see a doctor, remind them that a booster for the measles shot may be needed, and even offer to pay for flu and measles shots to encourage employees to voluntarily get these vaccinations. Doing any more presents a notable legal risk to employers, which are barred from discriminating on the basis of medical status under the Americans with Disabilities Act and on the basis of religion under the Civil Rights Act. Questions about immunizations could reveal both, as some forego vaccinations for religious reasons and others cannot get them because they are allergic, immunocompromised or have other complicating medical factors.
“The Americans with Disabilities Act generally prohibits employers from asking employees for medical information,” said Peter Gillespie, an attorney with labor and employment law firm Fisher & Phillips LLP. “By asking if they have been vaccinated or not, the employer risks invading their personal privacy by asking about issues that may otherwise have absolutely no relevance to the ability of people to do their job and that may be protected information under state and federal law.”
The safest course is simply to provide information, encouragement and incentives without questioning employees, he said.
In some instances where an individual may pose a direct threat to others, however, obtaining information about immunization status may actually be legally required. It is important to get guidance from local, state, CDC and federal authorities in those cases. When asking about immunization status is a legal requirement and there is a legitimate business reason, the EEOC will defer to the CDC and other agencies and not prosecute an employer for doing so.
But this does not necessarily mean that employers can require action. “In the case of an individual who is unable to get the vaccine, there may need to be accommodations that could involve having the employee wear masks or simply not deal with certain patient populations where the risk is present,” Gillespie said. “The employer still has an obligation to make an inquiry into the situation and deal with the facts that are present and make individualized determinations about the best course of action.”
In the event that an employee does become infected, employers must be careful when deciding how much to disclose to the rest of the office. The employee’s identity is likely considered private, and naming them may introduce ADA and HIPAA issues, depending on how the employer learned of the illness. For notification forms and letters, Gillespie recommends that organizations follow the lead of schools and day care facilities: disclose that there is a report of a sick person in the environment, inform the community at large so they can take reasonable precautions, and provide general information about the virus and recommendations on how to proceed. In most cases, that should be enough.
Safeguarding the workplace itself may demand more of the employer, particularly with the measles. “An employer faced with an outbreak has to think about what to do to protect the rest of the workforce,” Gillespie said. “Because the measles virus is a little bit heartier than a lot of others out there, it may be necessary to bring in someone to clean up an employee’s work station and the work area in general to make sure that the virus isn’t lingering somewhere on a doorknob, keyboard, coffee mug or other surfaces to which other workers are exposed.”
Beyond the ethical duty to keep workers safe, containing an outbreak is particularly important for employers to reduce the company’s broader legal liability. “If the exposure occurred in the workplace as a result of coming into contact with someone else in the workplace who had the illness, it may be a reportable event for purposes of OSHA recordkeeping,” Gillespie explained. “Depending on how the workers comp statutes are written, under state law, it may well be compensable under workers compensation as well.”
The liability cuts both ways, however. Specifically requiring vaccines or offering them could be a serious violation, while allowing employees to be infected due to insufficient precautions could also open the door to complaints, reputation damage and even lawsuits. The vaccine is extremely safe, according to every major medical organization, but employers that offer or require them might have to answer for any complications experienced by those who may already have a compromised immune system or preexisting condition, for example. “If an employer were to mandate vaccines and somebody has an adverse reaction, the employer could potentially be liable for forcing the employee to get the vaccine in the first place,” he said. “There may also be potential claims out there for negligent supervision depending on the employer’s awareness of what’s going on with an employee and if they’re allowed to return to the workplace.”
While Gillespie does not anticipate legal fallout from the current outbreak, he believes it presents a critical lesson for employers. “This outbreak is just another reminder to employers that these are policies that should be looked at and considered and employers should know where to get the information they need,” he said.
Much of that assistance can and should come from human resources, Gillespie said. “The human resources staff should have somebody who is keeping up to date on information relating to the various illnesses that are going around,” he said. “In most cases, the bigger risk to an organization is the disruption that comes about when you start to see something on the news and people begin to worry about their own situation and don’t necessarily have all of the information available. It is critical to have somebody within the organization who is looking to CDC for guidance and can help the organization assess the risks and relevant action to take on an individual, particularized basis.”
As with any virus, these prevention efforts can include having information available about the basic steps employees can take, from making sure that immunizations are up to date to reminders about hand-washing and other common-sense ways to keep from getting sick. “More often than not, the employer’s best measure to protect the workforce is simply to encourage everyone to take the reasonable steps to avoid picking up one of these viruses,” Gillespie said.
